
Viral and Plantar Warts
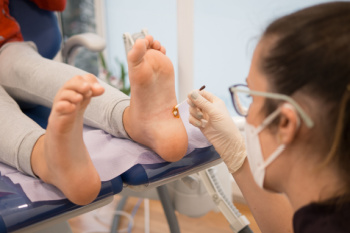
Viral and plantar warts are two foot conditions caused by the human papilloma-virus, abbreviated HPV. Viral warts, also known as common warts, typically appear as small, raised bumps with a rough texture on the surface of the skin. These warts can develop anywhere on the foot but are commonly found on pressure points like the heels or balls of the feet. Conversely, plantar warts specifically affect the soles of the feet, often appearing flat with a thickened callus-like texture and tiny black dots, known as wart seeds, within them. Both types of warts are contagious and can spread through direct contact or by walking barefoot in public areas like swimming pools or gym locker rooms. While viral and plantar warts are generally harmless and may resolve on their own over time, some cases may require specialized treatment to alleviate discomfort and prevent further spread. If you have developed warts on your foot, it is suggested that you visit a podiatrist who can effectively treat them.
Plantar warts can be very uncomfortable. If you need your feet checked, contact one of our podiatrists from Bruening Foot & Ankle. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our offices located in Covina and Alta Loma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Warts
Plantar warts are growths that typically appear on the heels or other weight-bearing areas of the feet. These warts are caused by the human papillomavirus (HPV). The virus enters the body through breaks in the skin, such as cuts, that are on the bottom of the feet. Plantar warts are more likely to affect children and teenagers, people with weakened immune systems, people who have a history with plantar warts, and people who walk barefoot in environments exposed to a wart-causing virus.
If you suspect you have plantar warts, you may have the following symptoms: pain or tenderness while walking, a lesion that interrupts the ridges in the skin of your foot, small fleshy lesions on the bottom of the foot, or a callus where a wart has grown inward over a well-defined spot on the skin.
HPV causes plantar warts to form and is very common. There are more than 100 kinds of the virus in existence. However, only a few of them cause warts on the feet. The other types of HPV are likely to cause warts on other parts of the body.
If you have plantar warts, your podiatrist may try different treatment methods depending on your specific case. Some treatments for plantar warts are peeling medicines (salicylic acid), freezing medicines (cryotherapy), or surgical procedures. Laser treatments and vaccines are also used to treat plantar warts.
The Definition of Tarsal Tunnel Syndrome
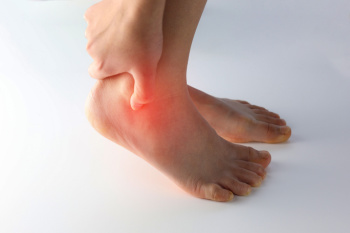
Tarsal tunnel syndrome, though less commonly known than other foot conditions, can cause significant discomfort and impairment for those affected. Similar to carpal tunnel syndrome in the wrist, tarsal tunnel syndrome involves compression of the posterior tibial nerve as it passes through a narrow space in the ankle called the tarsal tunnel. This compression can result from various factors, including injury, inflammation, or underlying conditions like arthritis or diabetes. Symptoms of tarsal tunnel syndrome may include burning pain, tingling, numbness, or weakness in the foot and ankle, often worsened by prolonged standing or walking. Left untreated, tarsal tunnel syndrome can lead to permanent nerve damage and functional limitations. Diagnosis typically involves a thorough physical examination, along with imaging studies like MRI or nerve conduction tests. Early recognition and intervention are critical for managing tarsal tunnel syndrome effectively and minimizing long-term consequences. If you have any of the above symptoms, it is suggested that you confer with a podiatrist who can offer you effective treatment solutions.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact one of our podiatrists of Bruening Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our offices located in Covina and Alta Loma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
Healing Time for Foot Stress Fractures
Suffering from a foot stress fracture can be frustrating and challenging, especially when it disrupts your daily activities and mobility. The healing time for a foot stress fracture can vary depending on several factors, including the severity of the fracture, your overall health, and adherence to treatment protocols. Generally, foot stress fractures take approximately six to eight weeks to heal, but in some cases, it may take longer for complete recovery. During this period, it is wise to follow your podiatrist’s recommendations diligently, which may include rest, immobilization with a cast or boot, and avoiding weight-bearing activities. Maintaining a healthy lifestyle with proper nutrition and staying hydrated can support the healing process. As tempting as it may be to return to normal activities, rushing the healing process can prolong recovery and increase the risk of re-injury. If you have a stress fracture, it is strongly suggested that you are under the care of a podiatrist who can offer you appropriate treatment options.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Bruening Foot & Ankle. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Covina and Alta Loma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Custom Orthotics For Ankle Stability

Step with assurance, thanks to enhanced ankle stability from orthotics! If you're active and on the move, Custom Orthotics are your ally for stronger, steadier ankles. They align your foot and ankle, reducing the risk of sprains and offering solid support for every stride. Don’t let instability hold you back. Try Custom Orthotics from our office, and discover unshakable confidence in every step!
Relieving Ball of Foot Pain From Wearing High Heels

High heels can add elegance and style to any outfit, but they often come with the uncomfortable side effect of pain in the ball of the foot. Fortunately, there are strategies to alleviate this discomfort and enjoy wearing heels more comfortably. This can begin by considering heels with a lower height or platform soles to reduce the pressure on the ball of the foot. Additionally, insert cushioned insoles or gel pads into your shoes to provide extra support and shock absorption. These inserts can help redistribute weight and alleviate pressure points, preventing pain and discomfort. Another helpful tip is to choose shoes with a wider toe box to allow more room for the toes and reduce crowding in the front of the shoe. Additionally, taking breaks from wearing heels throughout the day and stretching the feet and calf muscles can help relieve tension and prevent pain. If you enjoy wearing high heels and are experiencing pain in the ball of the foot, it is suggested that you consult a podiatrist who can provide you with additional relief tips.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact one of our podiatrists from Bruening Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our offices located in Covina and Alta Loma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why High Heels Are Not Ideal for Healthy Feet
It is no secret that high heels are uncomfortable to wear for long periods of time. Although beauty is pain, you should not sacrifice the health of your feet for a stylish heel. Wearing high heels can potentially cause many different foot conditions that may be avoided by wearing proper footwear.
The structure of high heels forces weight of your body to get shifted forward toward the ball of the foot. The higher the heel you wear, the more weight and pressure get shifted forward. The pressure that your toes may experience from wearing heels may lead to hammer toes, bunions, and ingrown toenails. Extra weight and pressure resulting from wearing heels may cause stress fractures. Furthermore, heels may cause pinched nerves which may result in Morton’s neuroma.
High heels are even more dangerous for people who are clumsy. Falling or tripping while wearing heels can cause an ankle sprain or twist.
What many people don’t know is that heels can also cause back and knee problems. In order for your body to stay balanced on heels, your spine has to sway unnaturally, which adds stress to your spine muscles. This may cause you to experience a sore lower back.
If you decide to wear high heels regardless of the risks associated with them, there are ways you can minimize their harmful effects. One way to reduce injury is to massage and stretch your legs at the end of the day. Stretching can prevent the Achilles tendons and calf muscles from becoming too tight. If you are simply looking for more height, wedges and platforms provide a better surface area to distribute the body weight across compared to thinner heels.
If you experience pain from wearing high heels, it is important to see a podiatrist before any of your symptoms become worse.
Orthotics for Children

Orthotics, also called orthotic insoles or shoe inserts, are customized flexible supports designed to correct specific foot imbalances causing pain or other issues. Orthotics can be worn by children as young as age two, but should only be prescribed by a podiatrist. Signs that a child may need orthotics can include in-toeing or out-toeing, or foot, ankle, knee, or leg pain. Other signs include tripping or falling frequently, abnormal gait, knock-knees, or significant lower body misalignment. If you are concerned about your child’s feet and think they might benefit from orthotics, it is suggested that you schedule an appointment with a podiatrist. This type of doctor can offer a proper assessment and monitoring to discuss if orthotics would be effective in addressing your child's foot issues.
Custom orthotics and shoe inserts are not just for cushioning the soles; they are about supporting the foundation of our body - our feet. The advantages extend far beyond immediate relief from discomfort. These personalized solutions, that Our doctors can prescribe, can significantly impact a person’s posture, alleviate pain in various parts of the body, and even enhance athletic performance.
As we lace up our shoes each day, having the right support can make a world of difference. Custom orthotics are like tailored suites for our feet, offering a bespoke solution to address our unique biomechanical needs. They provide stability where it is lacking, correct imbalances, and ensure that every step is a confident and pain-free one.
Custom orthotics and shoe inserts offer long-term health benefits. By addressing issues such as overpronation or underpronation, heel pain, plantar fasciitis, etc. orthotics can help prevent injuries and mitigate the progression of existing conditions. It’s an investment not just in the present, but in the future health of your feet and consequently, your overall well-being.
If you have any questions please contact our offices located in Covina and Alta Loma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.






